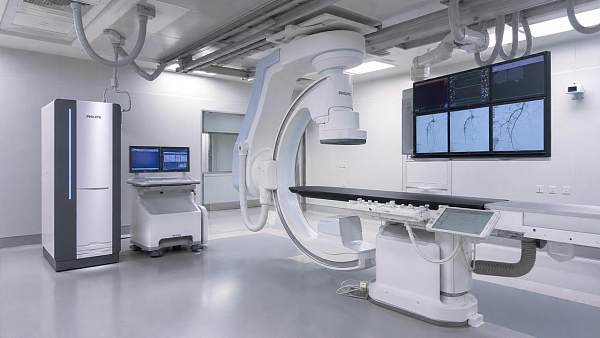
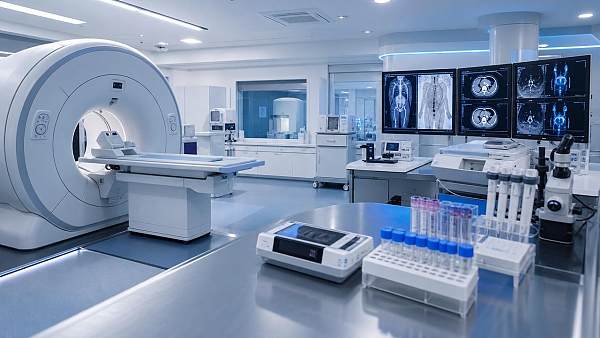
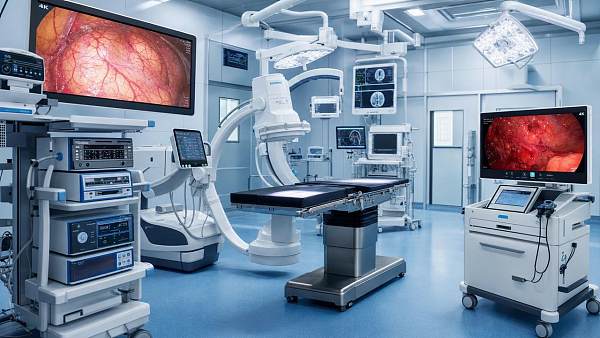
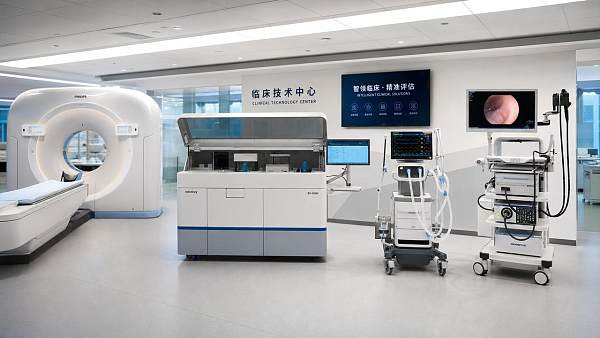
Why surgical imaging technology matters in complex cases
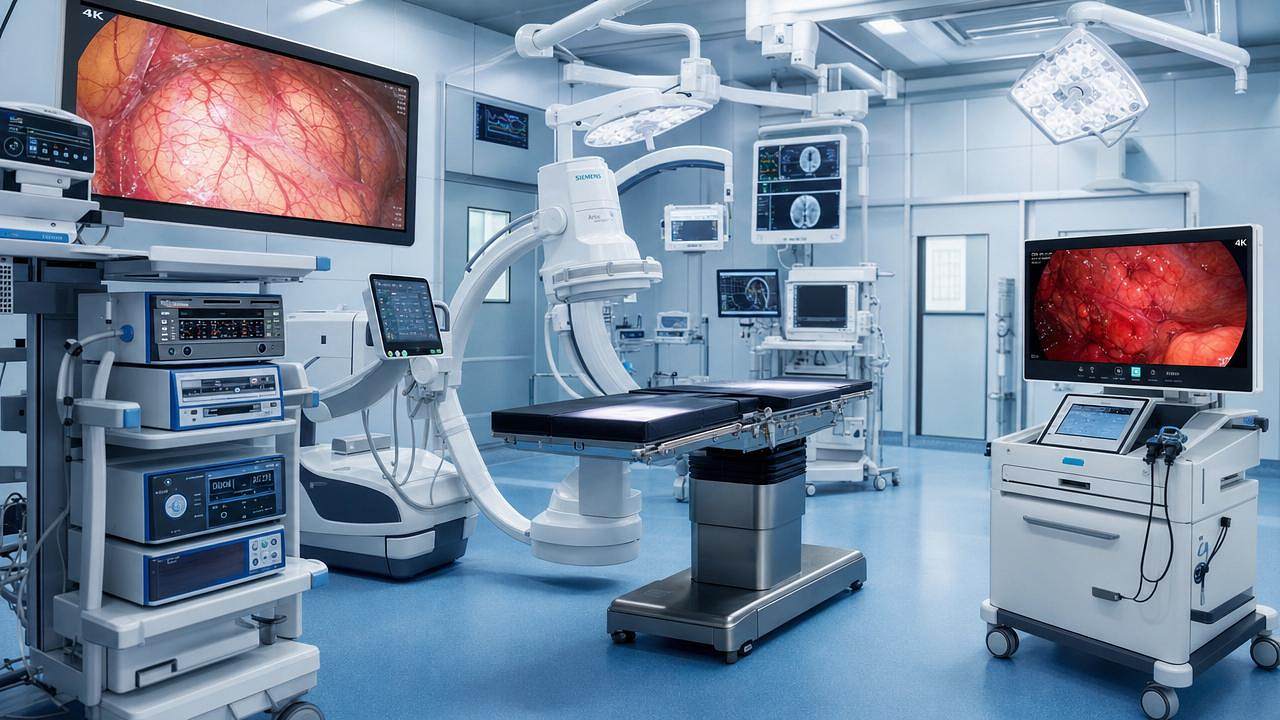
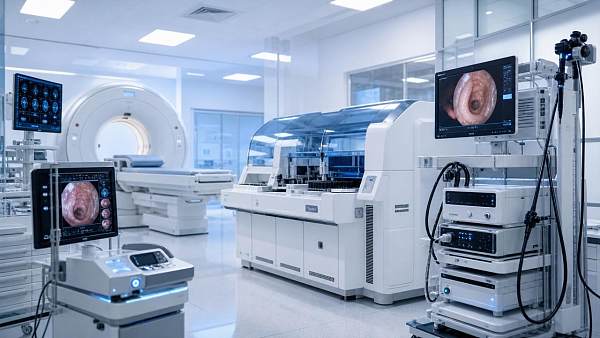
In complex procedures, surgical imaging technology is more than a visual aid—it is the operator’s real-time guide to safer decisions, clearer anatomy, and greater precision. From minimally invasive interventions to high-risk surgical workflows, advanced imaging helps teams reduce uncertainty, improve coordination, and protect patient outcomes when every second and detail matter.
Why does surgical imaging technology change outcomes in difficult procedures?
For operators, the value of surgical imaging technology starts with one practical reality: anatomy is rarely textbook-perfect in a live case. Tumors distort tissue planes, vessels may branch unpredictably, and prior surgery can leave dense adhesions that make orientation difficult.
In those moments, imaging is not a supporting accessory. It becomes the live decision layer between what the team expects and what is actually happening inside the patient. That difference matters most in neurosurgery, cardiovascular intervention, trauma, hepatobiliary surgery, and complex endoscopic work.
Modern surgical imaging technology also supports the broader digital operating room. It connects with endoscope systems, core OR infrastructure, navigation software, image reconstruction tools, and post-procedure documentation. For operators, this means fewer blind spots and better workflow continuity.
- It improves anatomical identification when the visual field is narrow, bleeding is present, or the lesion margin is unclear.
- It reduces repositioning and repeated instrument passes, which can lower procedural risk and save valuable OR time.
- It helps teams confirm placement, resection boundaries, drainage routes, and implant orientation before complications escalate.
- It supports communication across surgeons, anesthesiologists, radiology partners, nurses, and biomedical engineers.
At AMDS, this value is analyzed across the full MedTech chain. Surgical imaging is not treated as an isolated device category, but as part of a precision ecosystem linked to imaging diagnostics, minimally invasive tools, life support, OR infrastructure, compliance, and ROI planning.
Which complex scenarios rely most on surgical imaging technology?
Operators usually feel the importance of surgical imaging technology most clearly when visualization is limited, procedural margins are tight, or downstream consequences of misplacement are high. The use case should guide the system choice, not the other way around.
The table below summarizes typical high-demand scenarios and the imaging priorities that often drive evaluation.
The main lesson is simple: not every complex case needs the same imaging pathway. Operators should match image modality, resolution needs, mobility, latency tolerance, and OR integration requirements to the actual case mix.
Scenario-specific pain points operators often report
Across hospitals and surgical centers, users tend to face recurring challenges when the imaging setup does not fit the workflow.
- The image is technically acceptable but not stable enough under smoke, fluids, motion, or difficult angles.
- The system interrupts the sterile field because cables, positioning arms, or interfaces are cumbersome.
- The display quality is good, but integration with documentation, PACS, or navigation tools is limited.
- The technology is over-specified for the actual volume of cases, creating poor capital efficiency.
What should operators compare before choosing a surgical imaging technology solution?
Procurement often fails when teams compare only headline specifications. In real practice, surgical imaging technology should be assessed as a use-case tool, a workflow tool, and a compliance-sensitive asset. That means operators should compare both performance and deployment fit.
The next table highlights a more decision-oriented comparison framework for hospitals, ambulatory centers, and specialty surgical units.
This comparison approach is especially useful when a team must justify budget under clinical outcome pressure and financial scrutiny. AMDS frequently emphasizes this cross-functional view because image performance alone does not guarantee surgical value.
Key technical factors worth prioritizing
- Latency and response behavior. Even small delays can affect hand-eye coordination in delicate maneuvers.
- Optical stability under heat, moisture, fogging, and rapid movement.
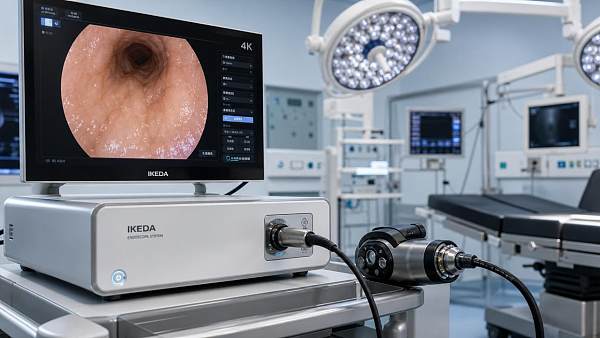
- Integration with 4K or 3D endoscope workflows where procedural depth judgment is critical.
- Ergonomics for prolonged use, especially in long and high-complexity cases.
- Data pathway readiness for recording, AI-assisted interpretation, and audit traceability.
How do budget, lifecycle cost, and alternatives affect the decision?
Price alone rarely explains whether surgical imaging technology is cost-effective. Operators and procurement leaders need to think in terms of total clinical utility: procedure volume, case complexity, downtime risk, training burden, accessory cost, and reimbursement logic all shape the real value.
A lower upfront option may appear attractive, but if image quality leads to slower workflows, more repeated steps, or narrower clinical use, it can become more expensive over time. This is where health economics thinking matters, especially under DRG-driven pressure.
- For low-volume centers, a modular or scalable configuration may offer a more practical entry point than a fully loaded platform.
- For tertiary hospitals, broader integration and uptime may justify higher capital spending because the cost of delay is significant.
- For ambulatory surgery settings, compactness, rapid turnover support, and easy sterilization workflow can outweigh premium imaging extras.
AMDS addresses these decisions by linking engineering detail with financial logic. That is particularly important when a buyer must explain not just what the system does, but why it matches the institution’s case mix, staffing model, and operating strategy.
Why do compliance and integration matter as much as image performance?
In medical environments, a strong imaging system still fails as a procurement choice if it complicates regulatory review, installation approval, or user adoption. Surgical imaging technology must fit the technical environment and the compliance environment at the same time.
Core compliance and deployment checkpoints
- Electrical and safety conformity documentation should be complete and consistent with the destination market.
- Instructions for use, labeling, cleaning guidance, and risk management files should support clinical deployment without ambiguity.
- Interoperability with hospital imaging archives, OR monitors, and adjacent device platforms should be checked before purchase, not after delivery.
- Installation planning should account for room layout, cable routing, display placement, power requirements, and sterile movement zones.
Because AMDS closely follows CE MDR, FDA expectations, diagnostic imaging trends, and OR integration pathways, it can help manufacturers and buyers translate compliance language into operational decisions. This reduces the common gap between engineering promise and clinical reality.
Common mistakes users make when evaluating surgical imaging technology
Some mistakes repeat across institutions, even experienced ones. Most are not caused by poor intent. They happen because evaluation is rushed, departments work in silos, or the team focuses on a single metric such as resolution or capital price.
Frequent evaluation errors
- Assuming better image specifications automatically mean better surgical usability.
- Ignoring operator ergonomics during long procedures and focusing only on procurement sheets.
- Underestimating service response needs in high-utilization operating rooms.
- Failing to verify compatibility with endoscope systems, OR lights, tables, storage, and data pathways.
- Treating compliance documents as a late-stage paperwork issue instead of an early selection criterion.
The safer approach is multidisciplinary review. Surgeons, nurses, radiology-linked stakeholders, biomed teams, and procurement staff should all contribute. Surgical imaging technology affects everyone in the room, so the selection process should reflect that reality.
FAQ: what do operators usually ask before purchase or upgrade?
How do we know which surgical imaging technology fits our case mix?
Start with your top procedures by volume, complexity, and risk. Then map the imaging demands of those procedures: field depth, motion sensitivity, need for real-time guidance, and integration with endoscopy or navigation. A center focused on advanced laparoscopy will prioritize different features than a spine or vascular team.
What should we prioritize when budget is limited?
Prioritize image reliability in your core procedures, compatibility with current OR infrastructure, maintainability, and staff usability. Avoid paying for advanced functions that your team will rarely use. In many cases, stable workflow performance brings more value than the highest available specification level.
Is surgical imaging technology mainly for large hospitals?
No. Large tertiary hospitals may need broader integration and advanced capabilities, but smaller surgical centers also benefit when precision, efficiency, and turnover matter. The key is right-sizing the solution to actual procedure demand and staff capability.
How early should compliance and documentation be reviewed?
As early as the shortlist stage. Reviewing market access status, labeling, safety documentation, and interoperability claims upfront can prevent delays during approval, installation, and commissioning. This is especially important for imported systems or cross-border procurement projects.
Why choose us for surgical imaging technology insight and selection support?
AMDS brings a rare combination of clinical technology observation, compliance awareness, and MedTech economics thinking. We do not look at surgical imaging technology as a standalone purchase line. We analyze how it connects with large-scale medical imaging, IVD-linked precision pathways, minimally invasive surgery systems, life support readiness, and core OR infrastructure.
If you are evaluating a new project, replacing legacy equipment, or aligning imaging tools with complex surgical growth, we can support practical questions that operators and decision teams actually face.
- Confirm technical parameters that matter for your procedures, including imaging behavior, workflow fit, and integration points.
- Compare solution paths for minimally invasive surgery, advanced OR environments, and cross-department imaging coordination.
- Discuss delivery planning, installation considerations, training expectations, and service readiness.
- Review certification and market access concerns relevant to target regions, including common CE MDR and FDA pathway questions.
- Explore customized recommendation logic based on procedure mix, budget boundaries, and expansion goals.
- Open quotation discussions with clearer technical and operational criteria, reducing rework during procurement.
When complex procedures leave little room for uncertainty, better imaging decisions start long before the operation begins. Contact AMDS to discuss parameter confirmation, product selection, compliance review, delivery timelines, or a tailored surgical imaging technology roadmap built around your real clinical workflow.
Recommended News
Weekly Insights
Stay ahead with our curated technology reports delivered every Monday.