Digital healthcare solutions can fail without this plan

Digital healthcare solutions can transform diagnosis, treatment, and care continuity.
Yet many programs stall after pilot launch or fail during scale-up.
The reason is rarely software alone.
Failure usually begins with weak planning across compliance, data, workflow, and accountability.
In complex clinical environments, digital healthcare solutions must support real decisions under strict timing and safety pressure.
That requires a plan linking engineering design with clinical operations and regulatory control.
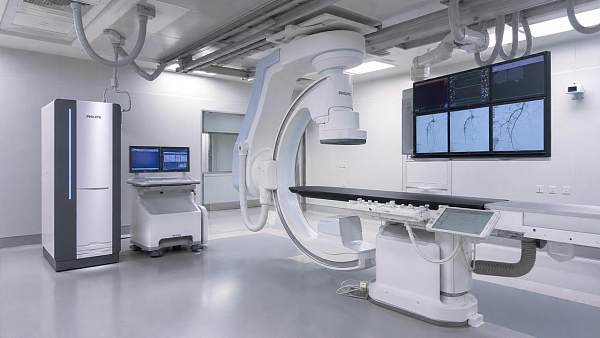
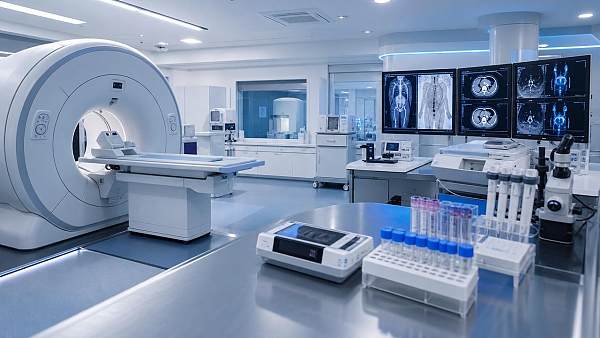
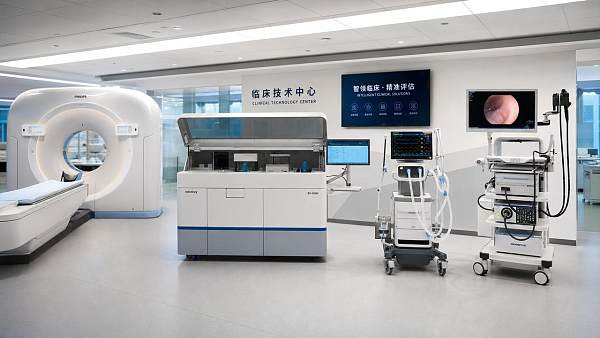
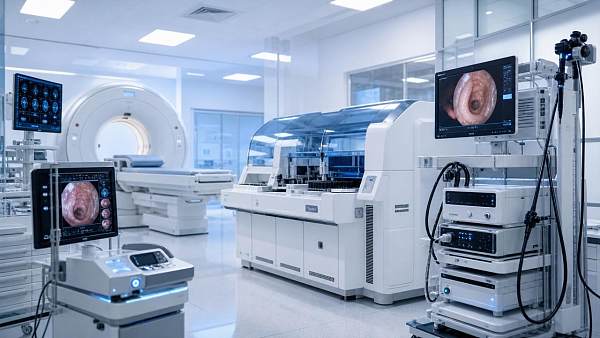
For organizations tracking medical imaging, IVD, life support, operating room systems, and endoscopy, this planning discipline is decisive.
AMDS observes this pattern across global MedTech markets every year.
The foundational plan behind reliable digital healthcare solutions

The essential plan is not a slide deck or procurement checklist.
It is an implementation architecture covering five connected layers.
- Clinical workflow mapping
- Data interoperability and governance
- Compliance and market access alignment
- Stakeholder ownership and training
- Scalability, security, and outcome measurement
When one layer is ignored, digital healthcare solutions become fragile.
A smart platform may still create unsafe handoffs, duplicate records, or delayed intervention.
In high-acuity settings, such gaps can cancel the expected value of digital transformation.
AMDS emphasizes this because advanced equipment no longer operates as isolated hardware.
Modern systems depend on stitched intelligence between algorithms, instruments, clinicians, and compliance frameworks.
Why digital healthcare solutions fail in real operating environments
Most failure patterns are operational rather than theoretical.
Teams often buy tools before defining the care pathway they must improve.
Integration planning is also underestimated.
A radiology platform may read images well but still fail to connect with PACS, RIS, EHR, or billing logic.
IVD data may be technically accurate yet unusable if result routing is delayed.
Life support devices may capture excellent parameters but create alarm fatigue if escalation rules are unclear.
Another common issue is compliance discovered too late.
If design controls, cybersecurity records, audit trails, or data privacy evidence are incomplete, deployment slows dramatically.
The result is predictable.
Digital healthcare solutions look innovative in demos but unstable in hospitals, laboratories, and surgical environments.
Frequent warning signals
Industry context shaping digital healthcare solutions today
The current healthcare market pushes digital healthcare solutions toward higher precision and stronger accountability.
This pressure is strongest in equipment-intensive clinical domains.
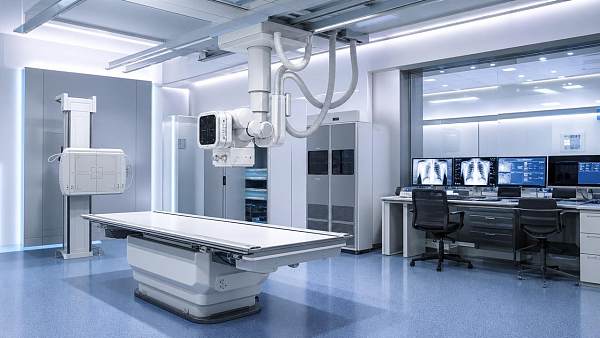
- Medical imaging requires algorithm transparency, image quality consistency, and interoperable reporting.
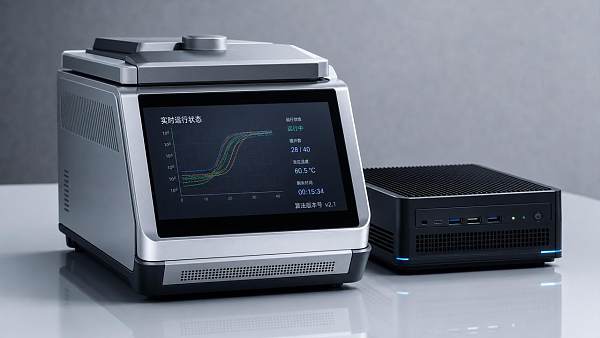
- IVD workflows require rapid turnaround, traceable samples, and reliable result communication.
- Life support systems require real-time monitoring, alarm management, and fail-safe continuity.
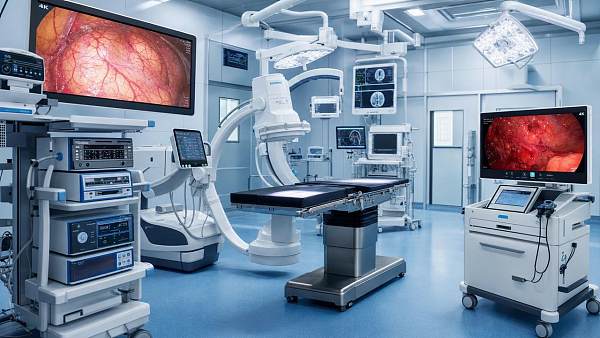
- Operating room platforms require precise device coordination and sterile workflow efficiency.
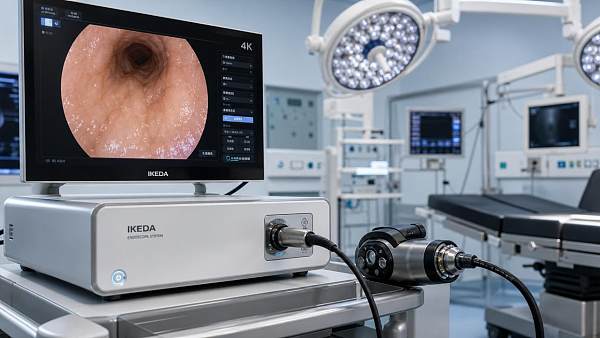
- Endoscopy systems require image fidelity, procedural documentation, and secure video data handling.
AMDS tracks these areas because each one combines technical complexity with heavy regulatory consequences.
As AI-assisted tools expand, the threshold for trustworthy digital healthcare solutions becomes even higher.
Organizations now need evidence of safety, efficacy, integration readiness, and economic value.
Business value created by well-planned digital healthcare solutions
A strong implementation plan protects both patient outcomes and business performance.
The operational gains are measurable when digital healthcare solutions are built around actual care pathways.
Core value areas
- Faster diagnosis through connected imaging, laboratory, and reporting systems
- Reduced rework through clean data exchange and standardized documentation
- Higher compliance confidence through planned validation and audit evidence
- Better clinical adoption through role-based workflows and practical training
- Clearer ROI through utilization metrics, downtime reduction, and reimbursement alignment
This matters especially for high-value equipment categories.
For example, advanced imaging systems depend on throughput, report quality, and service continuity.
IVD platforms depend on sample integrity, assay confidence, and fast communication loops.
Without coordinated planning, digital healthcare solutions may add cost without creating clinical leverage.
Typical implementation scenarios across clinical technology domains
The same planning logic applies across different healthcare technology environments.
These examples show why digital healthcare solutions need domain-specific execution details.
Generic deployment models usually miss critical clinical dependencies.
Practical planning recommendations for scalable deployment
A scalable program begins before software configuration.
It starts with disciplined planning decisions.
- Define the clinical event to improve, not just the tool to buy.
- Map every handoff between device, system, user, and patient record.
- Set compliance requirements at project start, including CE, FDA, privacy, and cybersecurity needs.
- Create measurable success baselines for time, accuracy, utilization, and risk reduction.
- Run workflow simulations before full launch in real-use conditions.
- Train by role, shift, and scenario rather than one-time generic sessions.
- Plan post-launch review cycles for defects, adoption gaps, and ROI evidence.
For advanced MedTech, these steps reduce friction between engineering ambition and clinical reality.
They also help digital healthcare solutions remain defensible during audits and procurement reviews.
Common oversight areas
- Ignoring legacy systems that still carry critical patient data
- Assuming AI output automatically fits physician decision logic
- Treating cybersecurity as an IT task only
- Measuring adoption by logins instead of clinical impact
- Missing service and maintenance implications for connected devices
A structured next step for stronger digital healthcare solutions
The most effective next step is a readiness review built around workflow, data, compliance, and economics.
This review should test whether digital healthcare solutions can perform under actual clinical pressure.
It should also confirm whether imaging, IVD, life support, operating room, or endoscopy systems can scale safely.
AMDS follows this evidence-led view across the global advanced medical equipment landscape.
The goal is clear.
Digital healthcare solutions should not only look innovative.
They must deliver precise, compliant, and scalable performance where health outcomes truly depend on them.
With the right plan, digital healthcare solutions become durable clinical infrastructure rather than short-lived pilots.
Recommended News
Related News
- 00
0000-00
Digital healthcare solutions can fail without this plan - 00
0000-00
How to compare advanced diagnostic systems before buying - 00
0000-00
Healthcare intelligence is reshaping smarter care decisions - 00
0000-00
How outdated hospital technology infrastructure slows care - 00
0000-00
What is driving medical equipment innovation in 2026?
Weekly Insights
Stay ahead with our curated technology reports delivered every Monday.