Digital Radiography ROI: When Upgrade Costs Start Paying Back
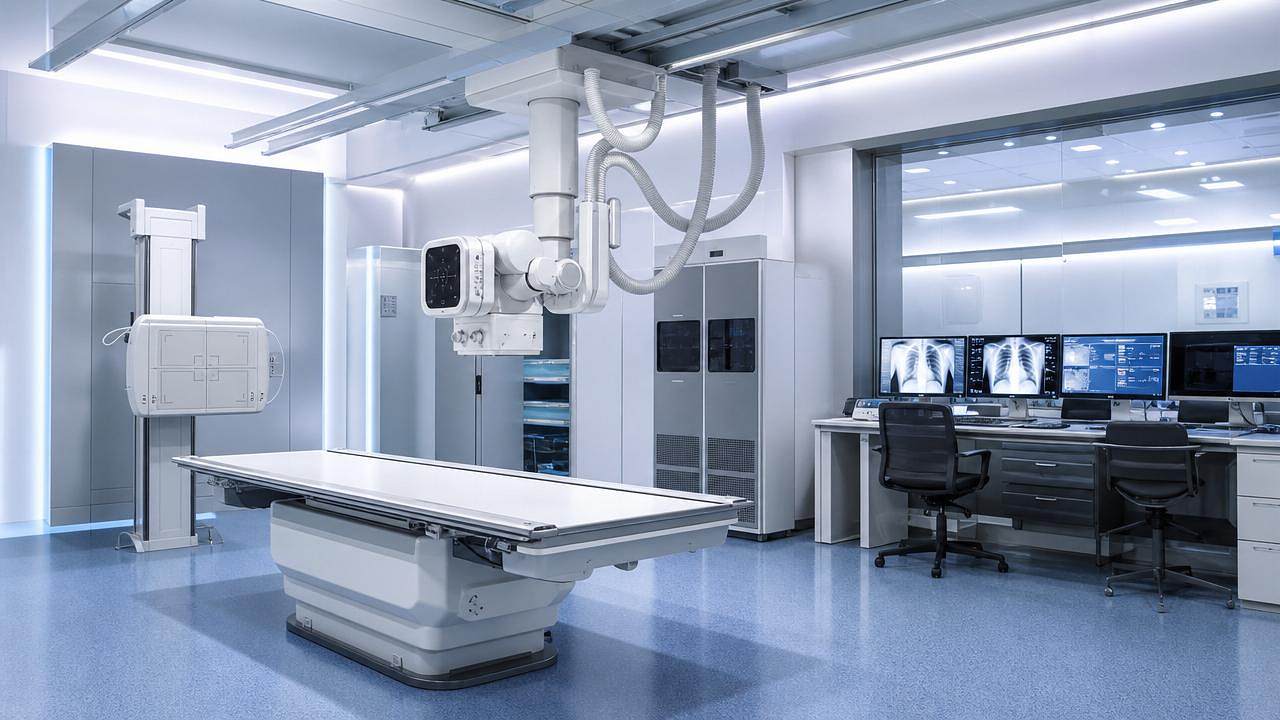
Upgrading to digital radiography is no longer just a technical decision—it is a business case. For commercial evaluators assessing medical imaging equipment, the real question is when higher acquisition costs begin translating into measurable returns through workflow gains, lower film and maintenance expenses, faster diagnosis, and stronger asset utilization. This article examines where ROI starts to emerge and what financial signals matter most.
For hospitals, imaging centers, and multi-site providers, digital radiography often sits at the intersection of capital budgeting, operational efficiency, and clinical throughput. The core challenge is not whether DR is better than film-based systems, but how quickly the upgrade improves cash flow, utilization, and decision quality.
For AMDS and commercial evaluation teams tracking medical imaging equipment, ROI analysis must extend beyond purchase price. It should include exam volume, retake rates, uptime, room turnover, service burden, staffing efficiency, and the speed at which imaging supports downstream diagnosis and treatment.
Why Digital Radiography ROI Emerges Earlier Than Many Buyers Expect
Digital radiography typically requires a larger upfront investment than computed radiography or legacy film workflows. Yet in many facilities, the payback window begins sooner than expected because several cost centers improve at the same time, often within the first 6 to 18 months after go-live.
The strongest return drivers usually come from four areas: consumables reduction, labor efficiency, faster exam cycles, and improved equipment utilization. These are especially relevant in outpatient imaging, emergency departments, orthopedics, and high-volume general radiography rooms processing 40 to 150 exams per day.
1. Film, chemistry, and storage costs disappear quickly
Film-based environments carry visible and hidden costs. Beyond film sheets and chemical processing, facilities must manage darkroom maintenance, disposal compliance, reprint waste, physical archive space, and manual retrieval. In medium-volume departments, these expenses can accumulate every month without improving diagnostic value.
When a facility shifts to digital radiography, these recurring costs decline sharply. While exact savings vary by geography and volume, business evaluators often model reductions across 5 to 7 cost categories rather than relying on a single line item such as film purchasing alone.
2. Faster workflow increases room productivity
A digital detector removes multiple manual steps. Technologists can review images within seconds, correct positioning sooner, and send studies directly to PACS or radiology workflow systems. In practical terms, even a 2- to 4-minute reduction per exam changes annual productivity materially.
If a room performs 60 exams per day, saving 3 minutes per exam creates 180 minutes of additional capacity daily. Over 250 working days, that equals 750 hours. Depending on scheduling strategy, this may support more same-day patients, shorter wait times, or lower overtime costs.
3. Retakes and image handling inefficiencies decline
Legacy workflows often absorb losses through repeat exposures, misplaced studies, manual labeling errors, and delays in image availability. Digital radiography does not eliminate retakes, but it usually improves positioning feedback and image consistency enough to reduce avoidable repeats and workflow interruptions.
For decision-makers evaluating medical imaging equipment, this matters because every unnecessary retake consumes technologist time, room availability, and patient cooperation. In high-throughput environments, cutting even 3% to 8% of repeat activity can support meaningful annual savings.
The table below shows where return usually starts to build in a digital radiography upgrade assessment. These figures are not universal benchmarks, but practical planning ranges often used in B2B equipment evaluation.
The key takeaway is that ROI rarely comes from one dramatic gain. It usually appears through stacked improvements across 4 to 6 operating metrics. That is why digital radiography can outperform a narrow capital-cost comparison when assessed as a workflow platform rather than a detector purchase alone.
Early warning sign of a weak business case
If a site runs fewer than 15 to 20 exams per day, has weak PACS integration, or lacks staffing discipline, the upgrade may take longer to pay back. In these cases, the technical merits of digital radiography remain valid, but the commercial return may shift from 12 months toward 24 to 36 months.
How Commercial Evaluators Should Build the ROI Model
A strong ROI model for medical imaging equipment should combine direct cost savings with capacity-based gains. Many evaluations fail because they measure only purchase price and annual service fees, ignoring throughput, utilization, and referral capture.
A practical model usually includes a 3-year and 5-year view, with sensitivity analysis for low-, base-, and high-volume scenarios. This gives finance, procurement, and radiology leadership a realistic range rather than a single payback claim.
Core cost and revenue variables to include
Commercial evaluators should capture at least 8 variables before comparing digital radiography proposals. Missing even two or three inputs can distort the decision, especially when detector quality, service models, and software integration differ across vendors.
- Acquisition cost, including detector, console, room retrofit, and installation
- Annual service contract and expected parts replacement cycle
- Exam volume per room per day, week, and year
- Average time per exam before and after upgrade
- Film, chemistry, archive, and disposal savings
- Retake rate and downtime assumptions
- Revenue or reimbursement per additional completed study where applicable
- Impact on referral retention, same-day access, and radiologist turnaround
Payback is often driven by utilization, not sticker price
A lower-priced system may appear attractive in procurement. However, if it has slower workflow, weaker detector durability, or limited integration with RIS/PACS, the total business outcome may underperform. In digital radiography, utilization quality is often more important than nominal discounting.
For example, a room operating at 55% utilization with frequent delays may not benefit from a low acquisition price if it still misses high-demand scheduling windows. A system supporting 10% to 20% more completed studies can justify a higher capital expense when demand already exists.
Three ROI calculation horizons that matter
Different stakeholders focus on different timeframes. Procurement teams often prioritize 12-month budget relief, finance may prefer a 36-month payback measure, and strategic leadership may look at a 5-year asset life with upgrade flexibility.
- Short term: 0 to 12 months, focused on consumables, installation disruption, and workflow stabilization
- Medium term: 12 to 36 months, focused on throughput, utilization, and service cost behavior
- Long term: 36 to 60 months, focused on lifecycle value, detector replacement risk, and digital ecosystem compatibility
The following table helps commercial evaluators compare digital radiography proposals using business-oriented decision criteria rather than technical specifications alone.
This comparison framework makes one point clear: the best-performing medical imaging equipment proposal is not always the least expensive one. The strongest candidate is the system that converts clinical demand into stable throughput with manageable service risk over several years.
Where ROI Starts Paying Back in Real Operating Scenarios
Digital radiography delivers different types of return depending on the care setting. Commercial evaluators should avoid generic assumptions and instead map ROI to actual workflow intensity, patient mix, and staffing structure.
Emergency and urgent care settings
In emergency departments, the value of digital radiography often appears first in speed. Image availability in seconds rather than minutes can improve triage, reduce bottlenecks, and support faster physician decisions. Even if reimbursement per exam is fixed, patient flow gains can be significant.
When exam demand is uneven but intense, shaving 3 to 5 minutes from common chest or extremity studies may prevent queue build-up during peak windows. That matters operationally, especially in facilities trying to reduce hallway waits and improve bed turnover.
Orthopedic and outpatient imaging centers
In ambulatory settings, ROI is often tied to scheduling density. If the center can add 4 to 8 extra appointments per day without extending staff hours, digital radiography may justify its upgrade cost far earlier than expected. This is particularly relevant where same-day or next-day access drives referral preference.
For orthopedic practices, image review speed also supports physician-patient consultation within the same visit. That reduces handoff friction and may strengthen patient conversion into treatment plans, procedures, or follow-up imaging.
Multi-site hospital networks
Across a hospital group, the business case often expands beyond one room. Standardized digital radiography platforms can reduce training variation, simplify service contracts, and improve fleet-wide reporting visibility. Central procurement teams may find value in harmonizing 3 to 10 rooms under a common workflow model.
In these environments, ROI also comes from management visibility. Leaders can compare room utilization, downtime frequency, and exam cycle time across sites, then adjust staffing or scheduling based on measurable operating data rather than assumptions.
Common mistake in scenario planning
A frequent error is using average annual volume without examining peak-hour congestion. Two sites with 18,000 exams per year can have very different ROI outcomes if one faces heavy morning compression and the other has evenly distributed demand. Digital radiography value often becomes most visible during those compressed operating periods.
Risks, Hidden Costs, and Practical Buying Guidance
Not every digital radiography project performs as planned. The main reasons are usually weak implementation design, under-scoped integration, unrealistic throughput assumptions, or unclear service accountability. Commercial evaluators should pressure-test the proposal before approval.
Hidden cost areas to review before purchase
- Room renovation requirements, power changes, shielding review, or table replacement
- Detector damage exposure and replacement pricing
- Training time for technologists, radiologists, and IT support teams
- Temporary productivity dip during the first 2 to 6 weeks after installation
- Interface development or PACS workflow adjustments
Five questions procurement teams should ask suppliers
- What is the expected uptime target, and how is service response measured?
- Which components have the highest replacement risk over 3 to 5 years?
- How long does implementation take from order to clinical go-live, typically 4 to 12 weeks or longer?
- What workflow evidence supports the claimed exam-time reduction?
- How will the system integrate with the existing digital imaging environment?
A realistic threshold for positive payback
In general, positive payback becomes easier to justify when the site has steady demand, reliable digital infrastructure, and a clear plan to use recovered time capacity. If the organization cannot convert faster workflow into more completed studies, shorter delays, or lower labor waste, ROI will be slower.
That is why the smartest buyers evaluate digital radiography as part of a broader medical imaging equipment strategy. Detector performance, room ergonomics, data flow, maintenance, and staffing all contribute to the financial result.
Digital radiography starts paying back not at the moment of installation, but at the moment improved workflow becomes consistent and measurable. For commercial evaluators, the most reliable indicators are lower recurring consumable costs, reduced exam cycle time, stronger room utilization, fewer avoidable repeats, and controlled service risk across a 3- to 5-year horizon.
For organizations assessing medical imaging equipment investments, AMDS supports a more rigorous view of clinical technology economics by connecting workflow reality, compliance context, and purchasing intelligence. If you are comparing upgrade paths, validating a payback model, or planning a multi-site imaging strategy, now is the right time to get a tailored evaluation framework.
Contact us to discuss your digital radiography business case, request a customized ROI checklist, or explore broader diagnostic equipment intelligence aligned with your procurement and growth priorities.
Recommended News
Weekly Insights
Stay ahead with our curated technology reports delivered every Monday.