How outdated hospital technology infrastructure slows care

Outdated hospital technology infrastructure does more than frustrate staff—it slows clinical decisions, weakens data visibility, and increases operational risk. In modern healthcare, every delayed scan, disconnected device, or unstable network can affect patient flow, safety, and financial performance. For organizations navigating digital transformation, understanding how hospital technology infrastructure shapes imaging, diagnostics, life support, and surgery is essential to building resilient care delivery.
What is hospital technology infrastructure, and why does it matter so much?

Hospital technology infrastructure includes networks, servers, storage, device interfaces, cybersecurity layers, and clinical software that connect care environments.
It also supports imaging platforms, laboratory systems, life support integration, operating room coordination, and endoscopy documentation.
When hospital technology infrastructure is modern, data moves quickly, devices communicate reliably, and clinicians act with greater confidence.
When it is outdated, hidden delays spread across the patient journey. Registration slows. Images take longer to load. Results arrive late. Alerts may fail.
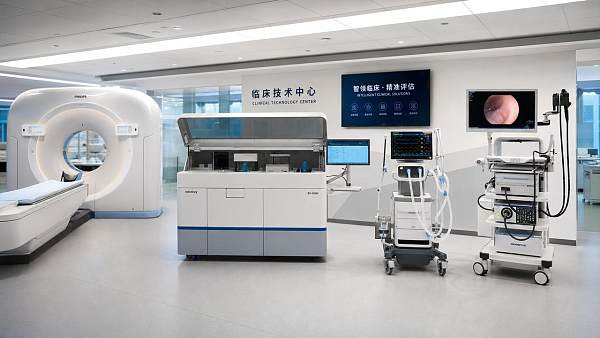
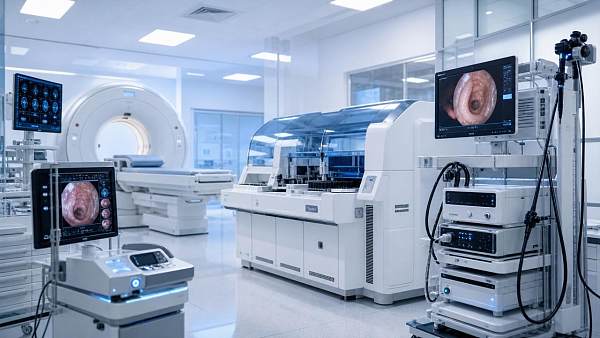
This matters across the broader medical ecosystem. Advanced imaging, IVD, critical care systems, and minimally invasive surgery depend on stable digital foundations.
AMDS closely tracks these dependencies because high-performance MedTech cannot deliver full value on weak infrastructure.
How does outdated hospital technology infrastructure slow diagnoses?
Diagnosis speed depends on how fast information moves from patient intake to test completion, interpretation, and clinician review.
Legacy hospital technology infrastructure often creates bottlenecks at each step. Systems may not integrate cleanly with RIS, PACS, LIS, or EHR platforms.
In medical imaging, outdated networks can slow large MRI or CT file transfers. Radiologists may wait for studies to render or reconstruct.
In IVD workflows, disconnected analyzers may require manual result entry. That adds delay, duplicate work, and transcription risk.
For urgent cases, even a short lag matters. Sepsis screening, stroke imaging, and cardiac assessment all rely on rapid data access.
Common diagnostic slowdowns linked to outdated hospital technology infrastructure include:
- Slow image upload, reconstruction, or archive retrieval
- Poor interoperability between instruments and core clinical systems
- Manual handoffs between departments
- Delayed result verification and clinician notification
- Downtime that forces temporary paper-based workflows
These issues reduce the value of premium diagnostic equipment. Fast scanners and precise assays still depend on reliable digital transport and storage.
Which clinical areas are most affected by aging systems?
The impact is strongest where complexity, data volume, and time sensitivity are highest.
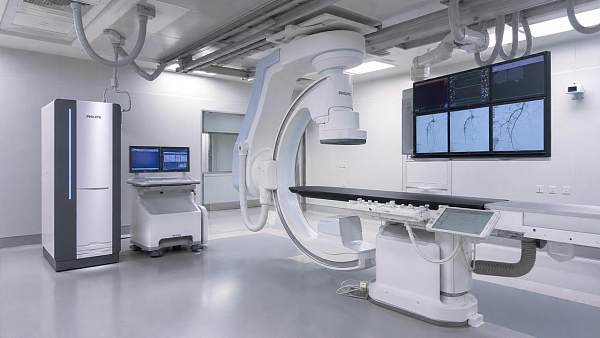
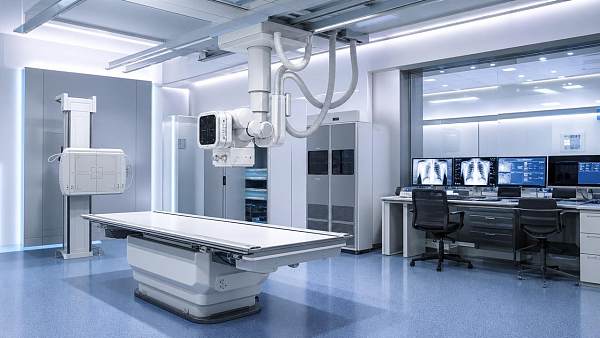
Medical imaging
CT, MRI, and advanced visualization generate large files and demand stable bandwidth. Aging hospital technology infrastructure can compromise throughput and reporting time.
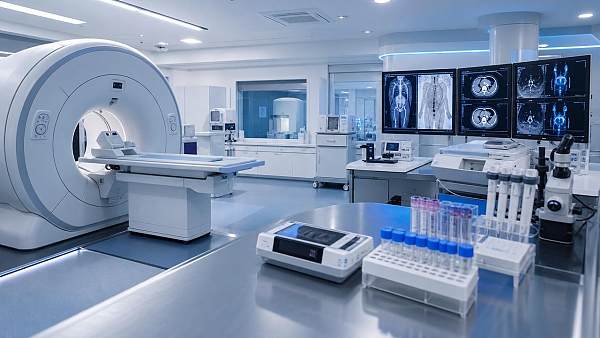
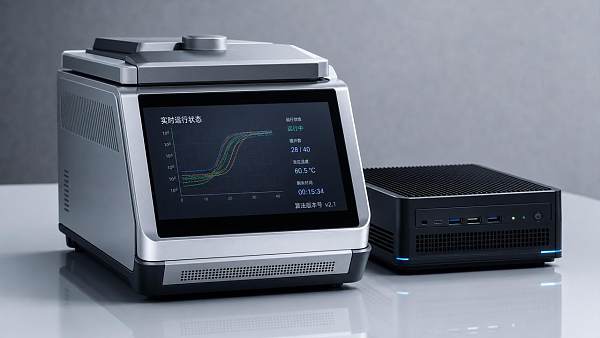
In vitro diagnostics
Modern IVD instruments produce actionable molecular and biochemical insights quickly. Legacy connectivity can block that speed from reaching bedside decisions.
Critical care and life support
Ventilators, monitors, and ECMO-related systems require dependable data capture. Inconsistent integration weakens trend visibility and alarm management.
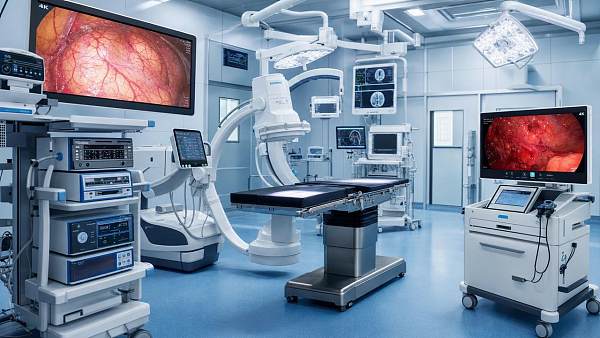
Operating rooms
Digital OR environments coordinate displays, imaging feeds, anesthesia data, and documentation. Old infrastructure increases setup friction and turnover time.
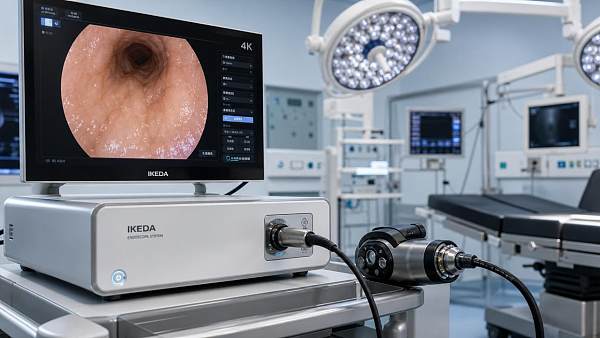
Endoscopy and minimally invasive surgery
4K and 3D systems depend on robust transmission and storage. Weak hospital technology infrastructure can degrade workflow continuity and data access.
Across all five pillars, the pattern is clear. Infrastructure is not a background utility. It is a clinical performance layer.
How can you tell whether hospital technology infrastructure is truly outdated?
Outdated systems are not defined only by age. They are defined by mismatch between clinical demand and technical capability.
Warning signs often appear in daily operations before they show up in strategic planning documents.
- Frequent delays accessing images or test results
- Repeated downtime or emergency workarounds
- Limited compatibility with new devices or AI tools
- Excessive manual data entry between departments
- Cybersecurity gaps and unsupported software versions
- Storage strain from growing imaging and video data
A simple test helps. Ask whether current hospital technology infrastructure supports faster, safer, and more connected care than three years ago.
If the answer is no, performance debt is likely accumulating.
What risks go beyond workflow delays?
Slow care is only one consequence. Outdated hospital technology infrastructure also affects quality, compliance, and long-term competitiveness.
Cybersecurity is a major concern. Unsupported systems create vulnerable entry points across networks connected to sensitive health data and critical equipment.
Compliance pressure also increases. Audit readiness becomes harder when data is fragmented, timestamps are inconsistent, or device logs are incomplete.
Financial leakage is another hidden cost. Delays extend length of stay, reduce room turnover, and underuse premium imaging or surgical platforms.
Innovation slows too. AI-assisted reconstruction, smart diagnostics, and integrated OR systems need a digital foundation that can handle volume and interoperability.
Without that foundation, organizations may buy advanced equipment but never realize the expected return.
How should modernization be prioritized without disrupting care?
The safest path is not a rushed replacement. It is a phased strategy tied to clinical bottlenecks and measurable outcomes.
Start with systems that affect diagnosis speed, patient safety, and interoperability. That often includes network performance, storage architecture, and core interface layers.
Then map infrastructure needs to the five major clinical pillars. Imaging, IVD, critical care, OR workflows, and endoscopy have different technical pressure points.
- Audit workflow delays by department and device type
- Measure downtime, result lag, and integration failures
- Prioritize cybersecurity and unsupported assets first
- Upgrade data pathways for imaging and diagnostics
- Plan staged implementation with rollback safeguards
- Track ROI through throughput, turnaround, and utilization
This is where strategic intelligence matters. AMDS emphasizes the link between compliance, engineering depth, and economic value.
A modernization plan should not focus only on replacing old hardware. It should enable precision diagnostics, safer intervention, and future AI adoption.
What does better hospital technology infrastructure look like in practice?
A strong hospital technology infrastructure is scalable, secure, interoperable, and designed around real clinical workflows.
In practice, that means high-speed image transport, seamless analyzer connectivity, reliable OR integration, and dependable support for life-critical systems.
It also means stronger visibility. Teams can trace data, monitor device performance, and identify friction before it becomes a patient care issue.
The result is not only faster care. It is a more durable operating model for precision medicine, compliance, and global MedTech competitiveness.
Outdated hospital technology infrastructure rarely fails in one dramatic moment. More often, it weakens care through small, repeated delays and missed efficiencies.
The path forward begins with honest assessment, targeted upgrades, and alignment between infrastructure investment and clinical priorities.
For organizations advancing imaging, diagnostics, life support, and minimally invasive surgery, stronger hospital technology infrastructure is not optional. It is the engine behind faster, safer, and smarter care.
Review where delays happen today, identify the systems creating them, and build the next upgrade around measurable clinical impact.
Recommended News
Related News
- 00
0000-00
Digital healthcare solutions can fail without this plan - 00
0000-00
How to compare advanced diagnostic systems before buying - 00
0000-00
Healthcare intelligence is reshaping smarter care decisions - 00
0000-00
How outdated hospital technology infrastructure slows care - 00
0000-00
What is driving medical equipment innovation in 2026?
Weekly Insights
Stay ahead with our curated technology reports delivered every Monday.