How interventional radiology equipment affects uptime
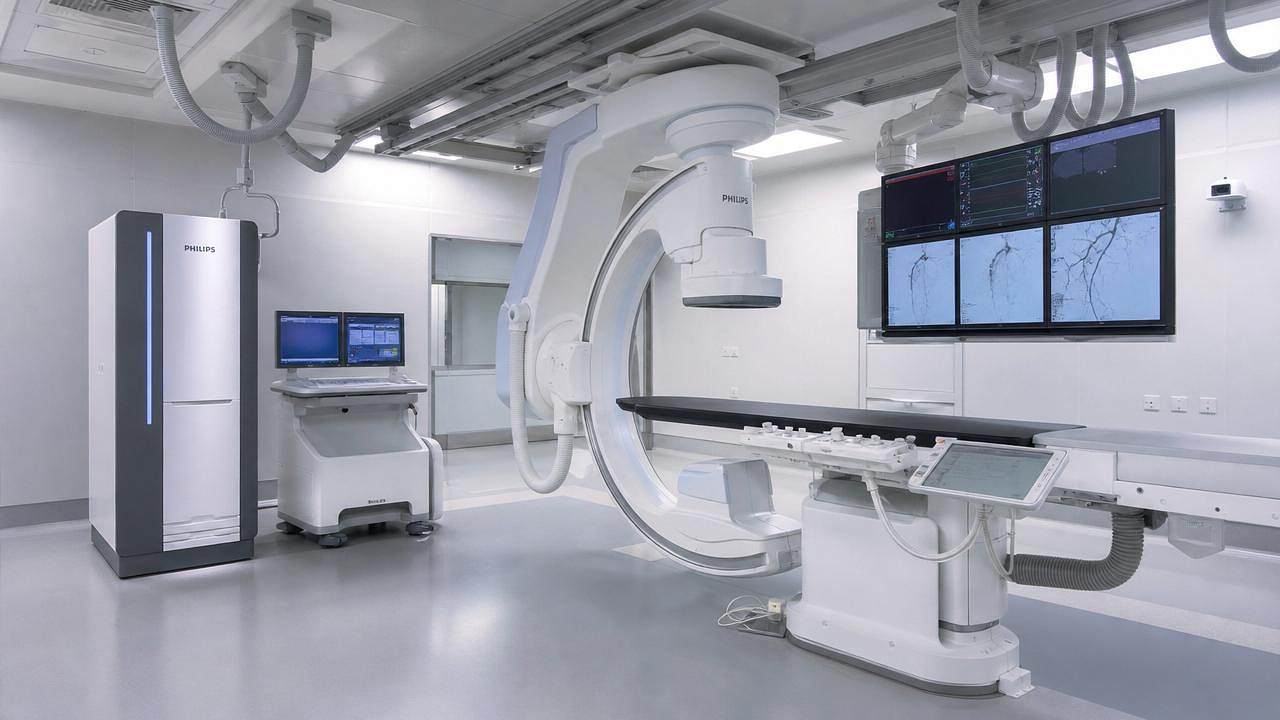
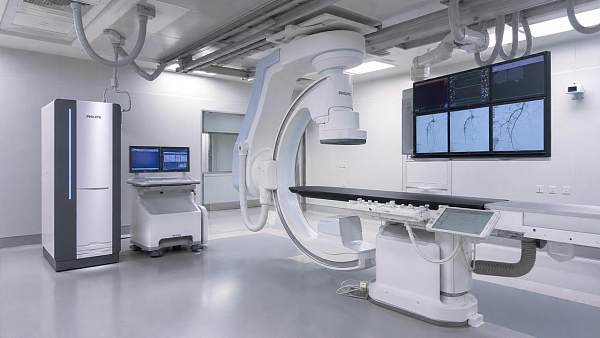
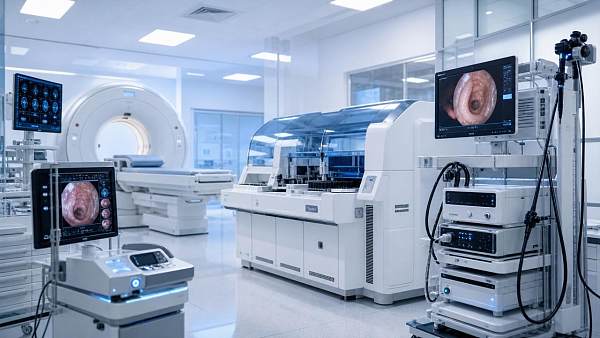
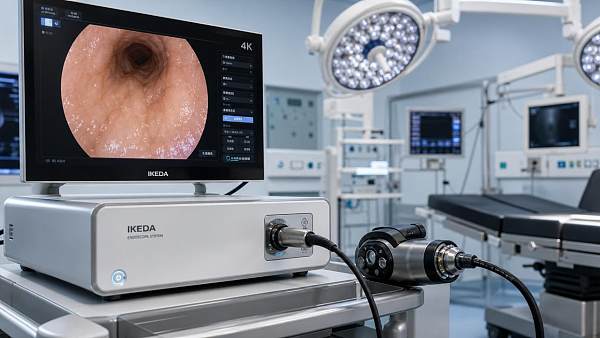
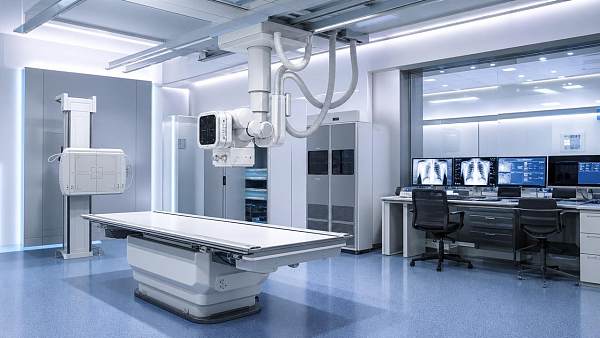
For service and maintenance teams, interventional radiology equipment directly shapes uptime, workflow continuity, and patient safety. From imaging chains and generators to detector performance and table motion systems, every component affects reliability under high procedural demand. Understanding how equipment design, serviceability, and preventive maintenance influence availability is essential for reducing downtime, accelerating repairs, and supporting consistent clinical performance.
Why does interventional radiology equipment have such a strong impact on uptime?
Interventional radiology equipment is not a single device. It is a connected clinical system with imaging, mechanics, software, power, cooling, and networking working together.
When one subsystem weakens, the whole procedure room slows down. Even minor faults can delay cases, extend patient preparation time, or force schedule changes.
This is why interventional radiology equipment affects uptime more than many stand-alone medical devices. It supports continuous, procedure-driven clinical operations.
In high-volume hospitals, uptime means more than technical availability. It also includes image readiness, predictable table movement, clean fluoro output, and stable software response.
A room can appear operational but still underperform. Slow boot cycles, detector artifacts, or gantry positioning issues can reduce usable uptime.
For AMDS, this links directly to the broader digital healthcare picture. Precision diagnostics and minimally invasive treatment depend on dependable equipment behavior.
Which components usually drive downtime?
- X-ray generators that drift under repeated load
- Flat panel detectors with artifact development
- Table motion assemblies with wear or calibration loss
- Cooling systems unable to manage long case sequences
- Control software with unstable updates or interface delays
- Cables, connectors, and power distribution points
Reliable interventional radiology equipment is therefore defined by system stability, not only image quality specifications on paper.
How do design and engineering choices influence serviceability?
Design decisions made early in product development strongly affect field uptime later. Serviceability begins with access, modularity, diagnostics, and documented maintenance pathways.
Interventional radiology equipment with modular detector units or isolated power boards can often be repaired faster than tightly integrated systems.
Built-in diagnostics also matter. Clear fault codes shorten troubleshooting and reduce unnecessary part replacement.
Remote monitoring adds another uptime advantage. Service teams can identify thermal trends, voltage instability, or software conflicts before visible failure occurs.
Mechanical accessibility is often underestimated. If replacing a drive assembly requires excessive disassembly, repair windows become longer and procedural disruption increases.
Software architecture is equally important. Interventional radiology equipment must support secure updates without creating compatibility problems across imaging, archiving, and navigation workflows.
What should be reviewed in design-related uptime planning?
- Time required to access high-failure components
- Availability of event logs and self-test records
- Swap-and-return versus bench repair strategy
- Software rollback capability after updates
- Cooling and power resilience during peak procedural loads
Well-designed interventional radiology equipment reduces not only repair time, but also uncertainty during diagnosis and scheduling.
What maintenance practices improve uptime the most?
Preventive maintenance is the most direct way to protect interventional radiology equipment uptime. However, routine tasks must match actual usage intensity and environment.
A fixed calendar alone is not enough. Rooms with dense vascular, oncology, or emergency procedures often need usage-based checks.
Critical maintenance actions include detector calibration, generator verification, table alignment checks, cooling inspection, cable wear review, and software health assessment.
Cleaning discipline also plays a hidden role. Dust accumulation, blocked airflow, and fluid exposure can shorten component life in interventional radiology equipment.
Another strong practice is trend-based maintenance. Repeated minor alarms often appear before a major service event.
When data is tracked over time, teams can intervene earlier, avoid emergency shutdowns, and align service with clinical downtime windows.
Recommended maintenance focus areas
How can teams judge whether interventional radiology equipment is truly reliable?
Reliability should be measured through operational evidence, not only brochure claims. The best review combines technical data, service history, and procedural fit.
Start with mean time between failures, mean time to repair, and repeat fault patterns. Then connect these metrics to room utilization and case complexity.
Interventional radiology equipment that performs well in moderate workloads may behave differently under intensive daily use.
Parts logistics are another deciding factor. Excellent equipment still creates downtime if key modules have long delivery cycles.
Support infrastructure matters too. Access to trained engineers, remote diagnostics, and validated spare inventory all affect real uptime performance.
Quick reliability checklist
- Does the interventional radiology equipment have transparent service records?
- Are common failure parts locally available?
- Can remote diagnosis shorten first response time?
- Do software updates follow controlled validation steps?
- Is performance stable during long, complex procedures?
This practical review helps distinguish nominal availability from dependable clinical readiness.
What are the most common uptime risks and misconceptions?
One common misconception is that newer interventional radiology equipment automatically means higher uptime. Advanced features may add performance, but also complexity.
Another mistake is focusing only on major failures. In practice, repeated minor faults often cause more workflow loss than one large breakdown.
Environmental conditions are also underestimated. Room temperature control, electrical quality, and cleaning protocols directly affect system stability.
Some organizations also delay maintenance to maximize daily case volume. This can create short-term gains but larger future outages.
A final risk is weak documentation. Without accurate service records, recurring issues in interventional radiology equipment remain hidden and root causes stay unresolved.
Risk comparison table
How should uptime planning connect with cost, compliance, and long-term value?
Uptime is not only a technical target. It also influences cost control, patient scheduling, regulatory readiness, and return on investment.
Interventional radiology equipment with unstable availability creates hidden costs through canceled procedures, overtime, rescheduling pressure, and emergency service calls.
Compliance is also affected. In highly regulated healthcare environments, poor documentation or unresolved performance drift can become audit concerns.
Long-term value comes from balancing acquisition quality, service support, maintenance planning, and operational visibility. The lowest purchase price rarely delivers the highest availability.
AMDS consistently observes that resilient clinical technology requires both engineering depth and service intelligence. This is especially true for interventional radiology equipment.
The most effective next step is simple. Audit current downtime causes, map them to subsystems, review maintenance intervals, and compare them with actual room usage.
Then prioritize serviceability, diagnostics, and spare readiness alongside image performance. That approach turns interventional radiology equipment into a stronger uptime asset.
When uptime strategy is treated as part of clinical quality, equipment decisions become clearer, repairs become faster, and procedure continuity becomes more dependable.
Recommended News
Related News
- 00
0000-00
How interventional radiology equipment affects uptime - 00
0000-00
Digital Radiography ROI: When Upgrade Costs Start Paying Back - 00
0000-00
Healthcare Data Analytics Is Only Useful if Imaging Systems Connect - 00
0000-00
How Accurate Is AI in Medical Imaging Outside Flagship Centers? - 00
0000-00
Medical Imaging Analysis Errors That Start With Bad Data
Weekly Insights
Stay ahead with our curated technology reports delivered every Monday.