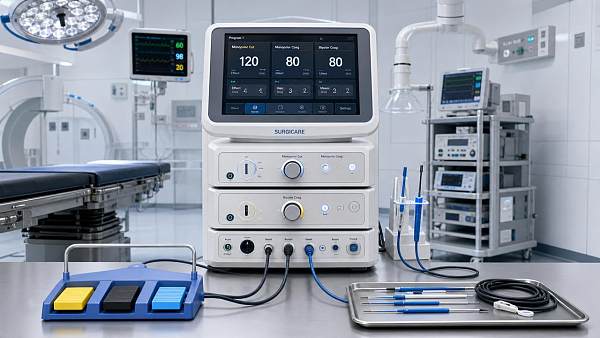
Electrosurgical Units: Cost Drivers Behind Service and Replacement Cycles
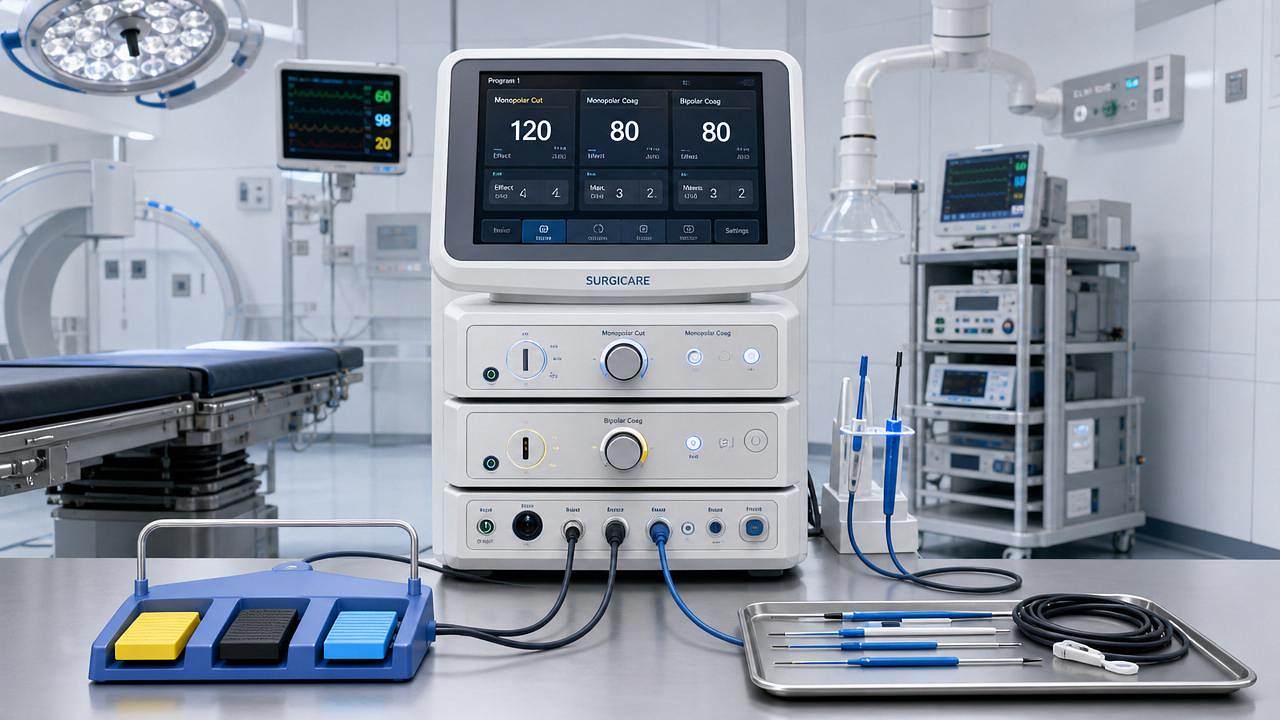
For financial decision-makers, electrosurgical units are more than routine capital assets—they are recurring cost centers shaped by maintenance, compliance, uptime, and replacement timing. In today’s operating room technology environment, understanding what drives service intervals and end-of-life decisions is essential for controlling budgets, reducing operational risk, and protecting surgical efficiency. This article breaks down the cost factors behind each stage of the equipment lifecycle.
What makes electrosurgical units a distinct cost category in operating room technology?
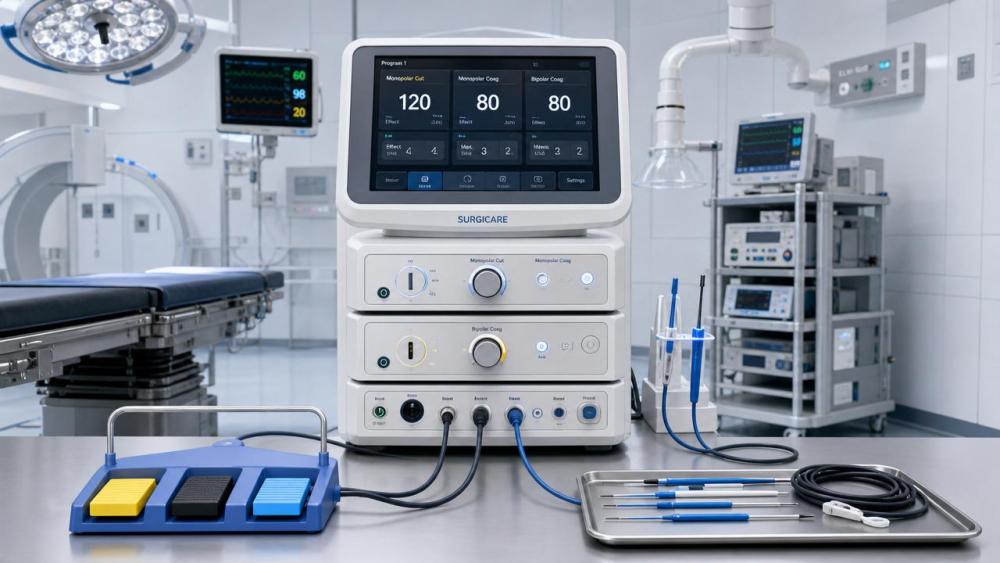
Electrosurgical units sit at the center of modern operating room technology because they directly affect tissue cutting, coagulation, and procedural continuity.
Unlike passive equipment, these systems combine generators, software, alarms, output controls, accessories, and safety monitoring.
That complexity creates layered costs beyond the purchase price. Service labor, calibration, accessories, and compliance checks all influence ownership economics.
In advanced operating room technology settings, electrosurgical units also interact with smoke evacuation, endoscopy platforms, and energy-based surgical workflows.
When one system underperforms, the effect spreads across scheduling, sterility turnover, case duration, and staff confidence.
This is why service planning should not treat the unit as a simple electrical box. It is a clinical performance asset.
- High utilization rates increase wear on connectors, footswitches, and output modules.
- Accessory compatibility affects both safety and ongoing supply costs.
- Regulatory testing intervals add predictable but unavoidable service expenses.
- Unexpected downtime can cost more than the repair itself.
Which factors usually drive service frequency and maintenance spending?
Service cycles are rarely determined by age alone. Usage intensity is often the strongest driver.
A unit used in back-to-back general surgery cases will need attention sooner than one reserved for occasional specialty procedures.
Environmental conditions matter too. Dust, fluid exposure, unstable power, and repeated transport shorten component life.
In operating room technology environments with multiple rooms, shared equipment often sees more cable stress and connector fatigue.
Common service cost drivers
- Preventive maintenance schedules required by internal policy or accreditation standards.
- Electrical safety testing and output verification.
- Software updates and manufacturer technical bulletins.
- Replacement of worn ports, switches, fans, and power supplies.
- Accessory-related failures caused by incompatible or low-quality disposables.
Another hidden cost comes from service response time. A lower annual contract may still cost more if repair delays interrupt surgical throughput.
For this reason, maintenance spending should be measured against uptime, not only invoice totals.
Strong operating room technology governance includes asset history, fault codes, service logs, and accessory failure tracing.
These records reveal whether costs come from normal aging or from workflow issues that can be corrected.
How do compliance, safety, and clinical risk affect replacement timing?
Replacement decisions often begin with risk, not age. An older unit may still function, yet no longer fit current compliance expectations.
Electrosurgical performance depends on stable output accuracy, alarm reliability, grounding integrity, and accessory recognition.
If any of these become inconsistent, risk rises quickly in high-acuity operating room technology environments.
A hospital may also face replacement pressure when manufacturer support ends. Parts scarcity changes the economics overnight.
Once boards, displays, or power modules become hard to source, repair costs increase and downtime becomes less predictable.
Signals that risk is overtaking service value
- Repeated output calibration drift between scheduled inspections.
- More frequent fault alarms during routine cases.
- Rising reliance on temporary fixes or borrowed units.
- Lack of cybersecurity or software support for connected functions.
- Incompatibility with updated smoke evacuation or safety systems.
In modern operating room technology, replacement is also driven by system integration needs.
Newer units may support workflow automation, better presets, lower thermal spread, and stronger event logging.
Those features reduce variance in performance and improve traceability, which matters during audits and incident reviews.
When is repair more economical than replacement?
Repair remains reasonable when failures are isolated, parts are available, and the unit still meets clinical and compliance requirements.
A single fan, connector, or footswitch issue does not justify replacement if uptime can be restored quickly.
The decision changes when recurring repairs start clustering. Multiple failures usually signal broader wear inside the platform.
A practical benchmark is to compare annual repair and contract costs against the expected remaining service life.
If yearly support approaches a large share of replacement cost, long-term value weakens.
Useful repair-versus-replace questions
- Is the failure limited to one module or spreading across subsystems?
- Can the manufacturer still guarantee parts and technical support?
- Will repaired performance remain stable for the next budget cycle?
- Does the current unit still align with operating room technology upgrades?
- What is the financial impact of one additional unplanned outage?
Repair analysis should always include indirect cost. A canceled case can outweigh a moderate replacement premium.
That is especially true in facilities where operating room technology utilization is tightly scheduled and turnover windows are narrow.
What hidden lifecycle costs are often missed during budgeting?
Many budgets focus on generator price and service contract fees. The larger lifecycle picture is often broader.
Accessory standardization, staff training, smoke management, and downtime contingency all change total ownership cost.
Operating room technology planning should include every touchpoint that supports safe electrosurgery, not just the base unit.
Frequently overlooked expenses
- Loaner equipment charges during long repairs.
- Training time when interface changes affect setup accuracy.
- Accessory waste from poor compatibility control.
- Workflow inefficiency from inconsistent presets or user confusion.
- Case delays caused by missing safety checks or cable failures.
Energy devices also influence adjacent investments. Better smoke control may reduce visibility interruptions in minimally invasive surgery.
That improves efficiency across the wider operating room technology ecosystem, including endoscopes, imaging displays, and insufflation systems.
How can lifecycle planning reduce cost without compromising surgical performance?
The strongest strategy is structured asset segmentation. Not every electrosurgical unit needs the same replacement timeline.
Units supporting complex or high-volume cases deserve tighter monitoring and earlier renewal thresholds.
Lower-acuity backup units may remain useful longer if they pass safety and output verification consistently.
This approach aligns spending with clinical impact and supports more disciplined operating room technology investment.
Practical steps for better lifecycle control
- Track repair frequency by room, procedure type, and accessory set.
- Separate preventive maintenance cost from emergency repair cost.
- Flag unsupported models before parts shortages become critical.
- Build replacement scoring around risk, uptime, and integration needs.
- Review electrosurgical performance alongside broader operating room technology modernization plans.
With this framework, replacement becomes proactive rather than reactive. Budgets become more predictable, and surgical disruption declines.
FAQ summary table: what should be checked before the next service or replacement decision?
Electrosurgical units remain essential to safe and efficient surgery, but their real cost is shaped by far more than acquisition price.
Service intervals, compliance pressure, integration demands, and downtime exposure all influence replacement cycles within operating room technology planning.
A disciplined review of asset history, support status, and procedural impact helps turn uncertain spending into predictable lifecycle management.
For the next step, build a decision matrix for each unit and compare repair trends against future operating room technology requirements.
Recommended News
Weekly Insights
Stay ahead with our curated technology reports delivered every Monday.